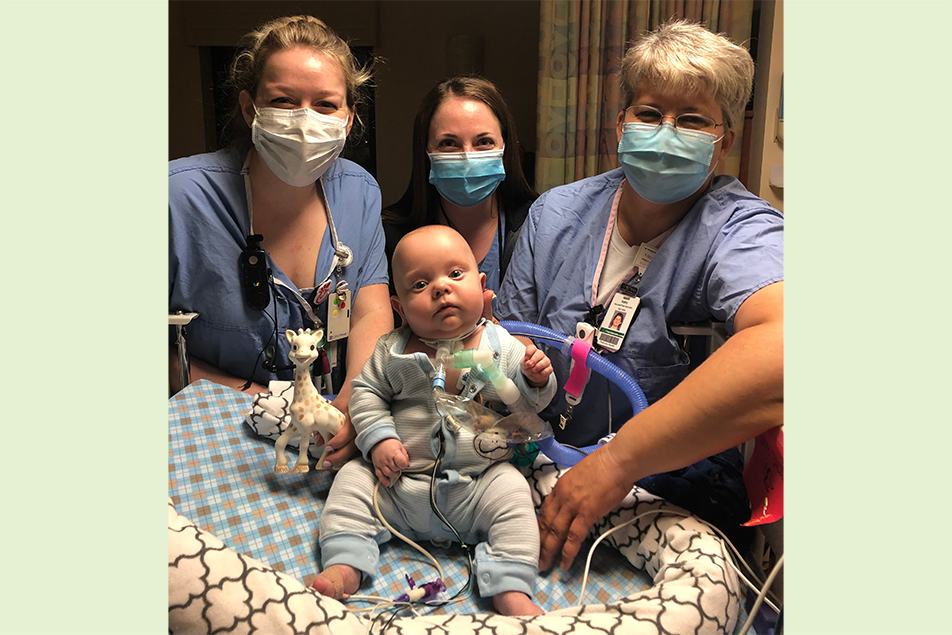
World Prematurity Day is celebrated to raise awareness of preterm births and their effects on families worldwide. According to the World Health Organization, an estimated 15 million babies are born preterm each year. To help shine a light on this critical health issue, we asked Kristi Reinhard, a former patient, to share the story of her son’s journey as a premature infant and the exceptional care they received.
What can you share about Silas’s health journey?
At 19 weeks, about halfway through my pregnancy, my water ruptured. Knowing it was way too early, we went in and found out there was no amniotic fluid around the baby. They told me to go home, take it as easy as possible, stay healthy, and hope and pray that I didn’t go into preterm labor or get an infection. To play it safe, I started quarantining at the beginning of February after my water broke. I didn't leave the house and we rarely had people into our home in hopes of avoiding getting sick.
Thankfully, our baby and I both stayed safe during that time. A few weeks later, on March 4, at 23 weeks gestation, I was admitted to Labor and Delivery at Parkview Women’s and Children’s Hospital to wait, hope and pray that I could keep our baby in utero for as long as possible.
Frequent ultrasounds continued to confirm the absence of amniotic fluid. Knowing that amniotic fluid is instrumental in lung development for a fetus, we walked a very uncertain path. Upon admittance, Ravi Kudumula, MD, PPG – Neonatology, came to speak with us. We discussed possible outcomes and what to expect if our baby was born before the due date. We had to take into consideration some of the most challenging questions we will ever have to face. These conversations were painful and challenging, but Dr. Kudumula was patient and compassionate toward us.
On top of what felt like an impossible situation, soon after my admittance, the hospital put COVID visitor restrictions into place. The only one who could visit was my husband, Jeremy. It was a lonely time. Jeremy had to balance taking care of our two girls, our home, and his career. I had to rest, stay healthy, and miss my kids at home.
Early morning on April 7, just shy of 28 weeks gestation, we welcomed our son, Silas, to the world by way of an emergency C-section. Just a moment later, a NICU team whisked my 2-pound 2.6-ounce baby boy away. I remember feeling a sense of relief but also dread. On the one hand, this long waiting period was over, but now we had to embark on another journey of the unknown. I felt joy but also grief. I had a baby boy, but I didn’t know if I would get to take him home with me.
Following Silas’s birth, we had to learn how to be parents all over again. Preemie parents. NICU baby parents. It felt like we were cramming for an exam, but we didn’t have the textbook, we’d never studied the subject before, and our child’s life depended on us succeeding. This is where our doctors and our nurses shined. They were so patient and took so much time with us, describing, explaining and teaching us what we needed to know. They never stopped encouraging us and speaking the truth about whether Silas had a good or hard day.
Silas was in critical condition for a while, but he was eventually moved off ventilation and onto a CPAP breathing machine as he stabilized. Around three weeks old, after that transition, I held my baby boy for the first time. They warned that being in the NICU can feel like being on a roller coaster ride. We knew there would be good days and bad days, but apart from a rocky first couple of weeks, Silas had a pretty steady incline and seemed to improve each day.
We were hoping to come home around his initial due date of July 1, but unfortunately, our sweet boy wasn’t ready. Silas still needed quite a bit of oxygen support and required a gastronomy tube (G-tube) to be placed because even though he loved eating from a bottle, he was silently aspirating food into his airway and lungs. After these adjustments, we planned to bring Silas home on July 31, but something still wasn’t right. His breath rate was too fast. He was expending all his energy on breathing. We made the hard decision not to discharge and instead stay and figure out what was going on.
In September, at five months old, Silas had a tracheoscopy surgery to allow the safe and effective delivery of oxygen to his lungs, helping him breathe more easily. After his trach surgery, Silas used his energy on things other than breathing, like staying awake longer and playing like babies are supposed to. The surgery was a difficult decision, but it was the right one for Silas and us. In October, after six and a half months in the NICU, Silas came home.
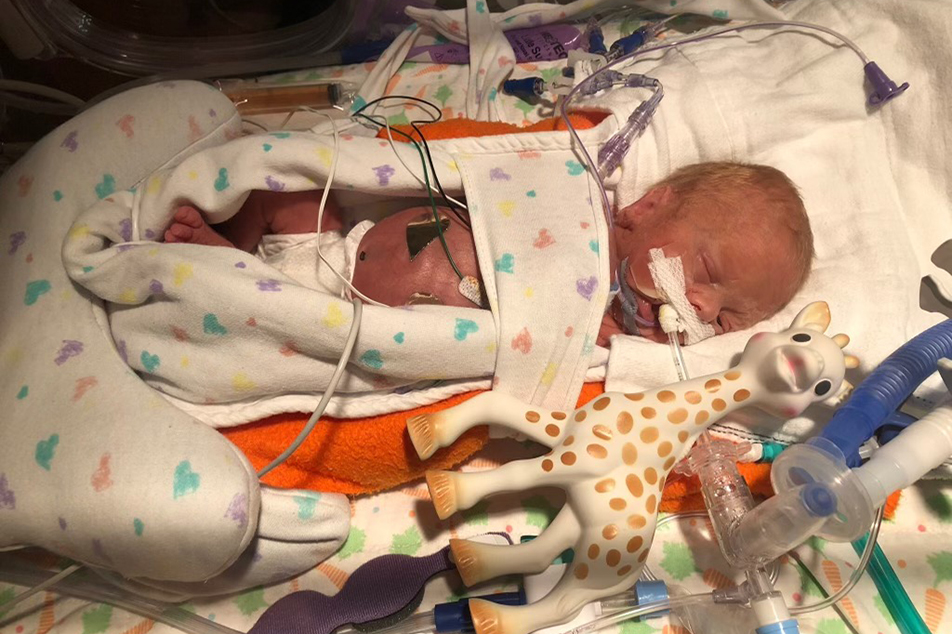
What role did the Parkview NICU team play in Silas’s journey?
It’s no secret that the NICU team have challenging jobs, but we saw firsthand what a fantastic group of individuals make up this team. They walked alongside us, supporting us through the scariest time of our lives, and they did so with compassion and grace. They were kind, encouraging, and patient, and they helped us hope in the middle of it all.
All six of the neonatologists that we worked with were outstanding. Each of them has an incredible ability to take a complex and nuanced situation and break it down so parents can understand it more clearly. I wish I had better words to describe them, but I hold them each in the highest esteem.
We were also privileged to work with many wonderful nurses and therapists. Their care and attention to detail were instrumental in Silas’s success. Everything we needed to know before bringing Silas home, we learned from this group of people. They answered questions, demonstrated care, pointed out things to look for, made us practice, practice, practice, all so we would be prepared to care for Silas at home as well as they cared for him at the hospital.
The NICU team not only saved our son’s life multiple times, but they became family to him and to us, which is way more than we could have ever asked for or expected. Every doctor, nurse and respiratory therapist did their jobs and kept him alive, but it was always much more than that. They cared for him and loved him. They are family, our NICU family.
What does this mean for Silas in the long-term?
For the moment, our goal is to keep Silas growing well with proper nutrition while trying our best not to let him get sick or contract an infection. Even in a world without COVID, bringing home a baby with Chronic Lung Disease during flu and respiratory syncytial virus (RSV) season is a tricky thing. But the hope is that we can keep him protected and healthy, and Silas will only have a couple of years or less of ventilation, then eventually be able to come completely off his trach and his G-tube.
As for the future, from what I understand, it could mean that nobody would ever know that Silas had a rough start to his life. Or it could mean he has asthma and probably won’t be an Olympic swimmer. Or it could mean he is an Olympic swimmer with a very cool story. No matter what, we are going to have hope.
What would you like to say to everyone involved in Silas’s care?
There’s no way I could ever say a big enough thank you. I’m filled with so much gratitude. There’s just too much appreciation and thankfulness that they were there, providing for my son when I literally couldn’t do it. I wasn’t enough for Silas, but the doctors, nurses and therapists were. They were everything to him.
What advice would you give other families going through a similar experience?
If you ever need a NICU, go to Parkview! When you are there, don’t be afraid to ask questions. Even if you think they’re not relevant or you’ve already asked them, ask them again. The staff is so kind, compassionate and happy to answer anything that comes to your mind.
Every person you interact with on that floor, from the moment you walk in the door to the moment you walk out, they care. They are all brilliant people, but they also have the heart for it. They care not only for the child but also the family. They also recognize that the child is the patient, but the family is an extension of that. I feel like they took as much care of me as they took of Silas.




