
We asked Bradley Hardin, MD, PPG – Cardiology, to share some recent findings and his thoughts on how alcohol consumption can impact cardiovascular health.
Patients come into the office all the time “armed” with the latest news and information they obtained from the Internet. Some of it is good data and helpful, while other content is less so. Alcohol use and its effects on the heart seem to come up quite a bit. As I like to say, “Ask 20 different cardiologists and you will get 30 different answers.” (Some of us will give you two or more answers). To start the discussion, let’s look at some of the recent data.
The latest study
In a recent study entitled “Alcohol-AF”, Alex Voskoboinik, MD, PhD, evaluated 140 patients who had atrial fibrillation (Afib) and described themselves as moderate drinkers, reporting an average alcohol intake of 16 drinks per week. He divided them into two groups: an abstinence group (those who stopped drinking) and a continued drinking group. Only 60% of the patients in the abstinence group were able to stop drinking completely, but most, roughly 86%, were able to reduce their intake by more than 70%.
The main endpoint of the study was this: The time to the first occurrence of Afib happened later in the abstinence group and was prolonged by 37% when compared to the group of continued moderate drinkers. The total amount of Afib was also decreased and over half of the patients in the abstinence group had 0% Afib compared to only 1/3 in the other group of the study. The study also looked at blood pressure and body mass index, both of which were statistically decreased in the abstinence group.
Of course, this was self-reported data on the amount of drinking as well as self-reported data on the amount of Afib. It’s common for the true amount of Afib to be higher when not self-reported.
The risks of alcohol consumption
Excessive alcohol intake is considered harmful to the heart. Alcohol increases your risk of Afib, high blood pressure (hypertension), obstructive sleep apnea, thickening of the heart tissue and a weak heart or cardiomyopathy.
Electrically, alcohol makes the heart tissue more “excitable” and more likely to develop Afib. Alcohol is loaded with carbohydrates, which contribute significant amounts of calories to a person’s diet and inevitably lead to obesity, a condition that can have many adverse downstream effects on the heart.
“Holiday Heart Syndrome” is a term referring to Afib occurring in the setting of binge drinking, either for habitual drinkers or rare drinkers. These symptoms can occur, not just on the night of or immediately after excessive drinking, but can be delayed up to 36 hours post-consumption, or in the “hangover” period.
In addition, chronic and/or excessive use of alcohol over sustained periods of time has been associated with autonomic dysfunction, which is how the body regulates blood pressure and heart function. For instance, if your autonomic system is damaged by alcohol, you may have chronic dizziness and an inability to maintain an upright position.
Gauging your intake
We grade alcohol intake as follows:
- Light – Less than 7 standard drinks* per week
- Moderate – 7-21 standard drinks per week
- Heavy – More than 21 standard drinks per week
*A standard drink is 14g of alcohol. [1] 14g of alcohol is around 12 ounces of regular beer (5% alcohol), 5 ounces of wine (12% alcohol), and 1.5 ounces of distilled spirits (40% alcohol).
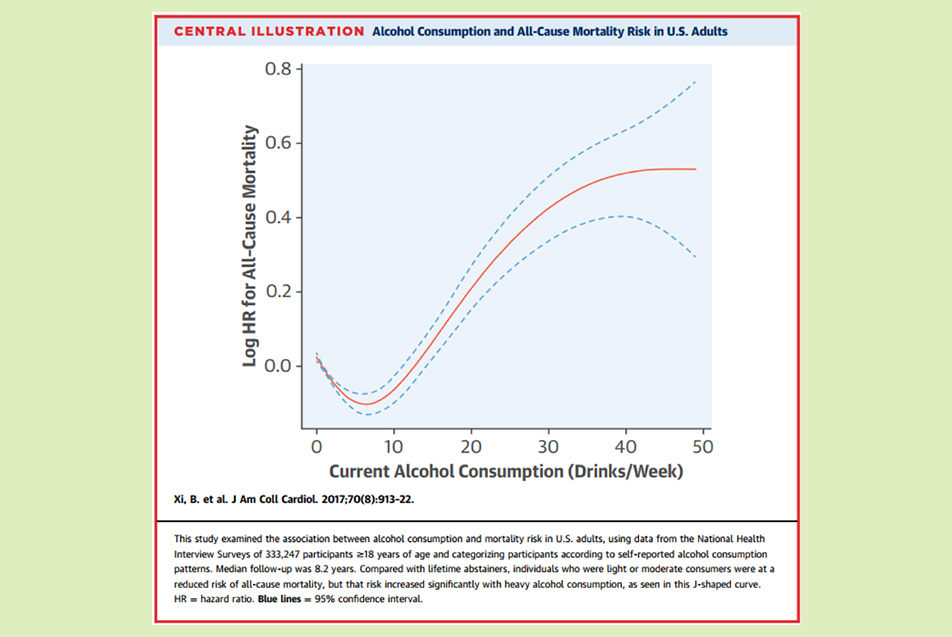
So, how much alcohol is safe for your heart? Like with many other things in life, it varies. Like I tell my patients, “Not everyone is built like a Chevy.” In general, one alcoholic drink per night for a woman and two for a man (men are typically heavier and have enzymes that metabolize alcohol better) is the limit. There is a definite J-shaped curve between alcohol consumption and death. Light use is probably associated with a lower risk of dying, but certainly, increased consumption has been associated with an increased risk of death.
Is one type of alcohol better than another?
There is no confirmed scientific support for this question. Some studies suggest that beer is less likely than wine or mixed drinks to increase your risk for Afib. Other studies say it makes no difference. Red wine is a great example. For years, scientists have described “The French Paradox”. The French seem to have a lower risk of ischemic heart disease, yet consume a diet high in saturated fats, cheeses, etc. Scientists proposed that their increased wine intake potentially offered protection against developing heart disease.
Red wine is thought to be protective because of resveratrol, which comes from the skins of grapes used in the wine. Other chemicals in wine, called polyphenols, are thought to be helpful in decreasing your body’s ability to form clots and increasing its ability to breakdown clots, as well as decrease inflammation in the body. In addition, they can decrease the adverse effects of LDL cholesterol or bad cholesterol. Interestingly though, when dealcoholized red wine (essentially grape juice) was studied, many of the same positive benefits were seen regarding heart health, as long as the flavonoids are not removed.
There are several studies that examine the heart-protective benefits of light to moderate alcohol intake (1-2 drinks per day). There is an association between light to moderate, continuous consumption of alcohol and reduced risk of developing coronary artery disease. However, this benefit disappears if there is acute or excessive use of alcohol. In that case, sustained heavy use or binge drinking actually harms the patient, by increasing the risk of arrhythmias, stroke and sudden death.
The American Heart Association notes that moderate consumption of alcohol (less than or equal to two drinks a day for men and less than or equal to one drink/d for women) is associated with a reduction in risk for ischemic heart disease. However, the AHA does not comment on whether one particular type of alcoholic beverage is more favorable.
The big takeaways
From an arrhythmia standpoint, less is more. Less alcohol means fewer arrhythmias. From a coronary artery disease perspective, light to moderate alcohol intake may slightly reduce your risk of having a heart attack and buildup of blockages in the heart.
Moderation seems to be the key. Binge drinking or excessive alcohol intake have both consistently been shown to cause harm with no positive benefits. The use of alcohol “to protect the heart” must be balanced with the adverse effects alcohol has on other organs in the body, mainly the pancreas and liver. Keep in mind, excessive alcohol use is also associated with increased domestic violence and injury while operating a car or other machine.
No studies exist that have shown that there is any “harm” to a person by not ingesting alcohol. So, if you don’t drink alcohol, you don’t need to start. However, if you are going to partake, then light to moderate drinking does not appear to be harmful to the development of coronary artery disease. Remember to practice moderation and know the risks before you drink.
Sources
[1] Voskoboinik et al. Alcohol and atrial fibrillation: a sobering review. J Am Coll Cardiol. 2016;68(23):2567-2576.
[2] Saheeb S, Alexander B, Baranchuk A. Wine and cardiovascular health: a comprehensive review. Circulation. 2017;136:1434-1448.



