This post was written by Courtney Leach, Digital/Social Media Manager, Parkview Health
On a Wednesday night, a little past bedtime, my three young daughters gathered around me for our evening reading ritual. We’re currently working our way through “Good Night Stories for Rebel Girls: 100 Tales of Extraordinary Women” by Elena Favilli and Francesca Cavallo. The pages are filled with the heroic tales of writers and activists, computer scientists and athletes, all female, all revered for blazing a path closed to others before them. All simply entertaining the voice inside them that said, “Of course you can. What else would you do?” I turned to a page with a faded illustration of Florence Nightingale. At the bottom, it read “I attribute my success to this – I never gave or took any excuse.”
We read a few more pages and I tucked them in tightly with thoughts of the tireless nurse, Marie Curie and Ruth Bader Ginsburg, among others. I kissed each one, pulled the covers up under their chins and went back to my room to prepare for the day ahead.
The next morning, just before 8 a.m., I stood in the surgery waiting area on the second floor of Parkview Regional Medical Center. Brandon Emry, NP, PPG – Neurosurgery, came around the corner and, without breaking stride, motioned for me to follow him back toward the Intensive Care Unit (ICU).
We passed by the nurse’s station and pressed our backs against the wall, opposite a patient’s room, where we could hear Stephanie Falatko, DO, PPG – Neurosurgery, inside. As we waited, I turned and whispered to my tour guide, “Have you been working with Dr. Falatko long?”
“I’ve only been her NP since April,” Brandon said, “but I worked with her before that, too. I was on one night and I met her and really enjoyed working with her. She’s fairly new and needed an NP, so it just fell into place.”
“Did you ever imagine you’d be in neuro?” I countered.
“No! Neuro is hard; every patient is different and it’s intimidating to work with someone who’s so intelligent. I have to rise to that every day.”
After several minutes, Dr. Falatko pushed back the curtain and emerged from the dark space behind her. We exchanged pleasantries as she grabbed her bag brimming with neurology and vascular texts ("You don't part with such friends after 15 years," she later told me) on our way to Interventional Radiology. She talked about her daughter – Nora, who’s 6 – and I mentioned my own girls. She’d been at the hospital until midnight last night, and was silently pleading with the coffee perched in her hand to carry its weight today.
8 a.m.

For this first case, Dr. Falatko was checking on the patient’s aneurysm using angiography, a method for capturing images where contrast is injected into the blood vessels before taking the necessary X-rays. This particular woman had an aneurysm in her brain that bled, resulting in a stroke. The aneurysm had been treated with a technique called coiling, a treatment in which the aneurysm is stuffed with tiny metal coils to seal it off to prevent it from bleeding again. Dr. Falatko would compare previously taken magnetic resonance angiography (MRA) images against the new angiography images, to determine whether blood was flowing through the coil, which could indicate that the aneurysm was not completely sealed off from the blood supply.
The neurosurgeon often uses conscious sedation for these methods so she can constantly check in on the patient, as was the case with this individual.
“Can you wiggle your toes for me? Good. Now squeeze my hand. Great. Show me your teeth,” she directed, leaning down near the patient’s face.
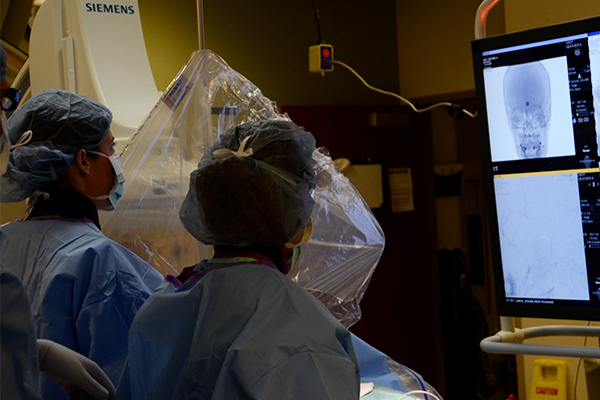
Unlike a simple point and click, capturing these images was a far more complicated process. After a few initial shots, a map of what looked like sprawling tree roots – blood vessels in the brain – appeared in one of the six squares on the giant screen in front of the operating table. Her eyes would stay here for the next hour. She asked someone to read off the numbers she wrote on a piece of paper earlier that day. Coordinates, I thought. I would learn she was plugging in areas that correlated to the best views for looking at the coiled aneurysm; intersections of the A plane and the B plane. Her goal was to see the aneurysm under the highest magnification to see if blood was entering around the coils.
In order to position her patient to hit the target, she had to maneuver just so. She drove the mechanical table like an expert coder, bumping the levers to the right, tapping switches to the left, pushing pedals in quick, punchy spurts. She waited until the patient was in the exact spot for the beam to pass over the intersecting planes and then announced she was “firing”.

“Don’t move, don’t breathe, don’t swallow. You’re doing great, honey. It’s going to be over soon.”
“Thank you for everything,” the patient responded. “You saved my life.”
“I’m just the vehicle,” Dr. Falatko said.
She excused herself to go take a closer look at the colorful images coming up on a monitor in the staff area just off the procedure room. The rich hues on the screen began at the brain stem and saturated the contrast driven pathways like a beautiful crimson ink.
Not quite satisfied, Dr. Falatko came back for a few more images to confirm her diagnosis, talking her conscious patient through it, every step of the way.
“You will feel some warmth, OK? That’s normal. Maybe some dizziness ...”
She noticed some blood supply to the coil, which, as she told her patient’s waiting spouse just minutes after completing the angiography, could just mean the aneurysm needs more time to clot. Though, she suspects she will eventually have to treat the aneurysm. A decision to weigh another day.
9:15 a.m.
We visited Dr. Falatko’s next patient, who required a stent. This, too, would be conducted under conscious sedation so she could monitor his neurological activity.
“I’m going to go through the leg, cross the narrowed area, deploy an umbrella-like tool past the narrowing to prevent blood clots from going into the brain, insert and blow up a balloon, and then place the stent in the carotid artery across the narrowing. Finally, I’ll take the umbrella out. Does anyone have any questions?” And, even though her pager was sounding in Brandon’s hands just an arm’s length away, she answered each one, thoughtfully and evenly.

During the morning’s angiography, a possible stroke patient had arrived in the Emergency Department. Now, Dr. Falatko began rapidly running through a series of questions as we walked toward the patient’s room. When we arrived, she wasn’t there. We stopped into the CT area. We’d just missed her. We went into MRI, where Dr. Falatko was finally able to offer an evaluation and confer with the caregiver currently accompanying the patient.
“We want to look at perfusion,” Brandon explained to me off to the side. “Different colors in the scan will show how long it takes the blood to move through.”
Strokes can be attributed to a disruption in the normal cerebral blood flow. They are also commonly attributed to high blood pressure and other medical problems, such as uncontrolled diabetes and high cholesterol, though smoking certainly doesn’t help either.
10 a.m.
We put our lead back on and returned to the Interventional Radiology procedure room where Dr. Falatko would place the second patient’s stent.
“He has 80-90 percent stenosis (abnormal narrowing of a passage) and we want to get that to 40-50 percent,” she explained as she pushed her arms through the paper surgical gown.
The multi-step process involved threading a line in from the femoral artery, right above his hip, up to his carotid artery in his throat, then inserting an umbrella-like structure to catch any debris, then a balloon, which would push out any obstructive plaque before the doctor was able to place the stent. For more than two hours, Dr. Falatko repeatedly ran through her checklist: “Can you wiggle your toes for me? Good. Now squeeze my hand. Show me your teeth,” she said, leaning down near his face.
She took several images first to create her roadmap, an intricate display of vessels and pathways. The line she placed first was like a tube or a tunnel, the passageway through which she would deliver all of the necessary pieces to secure the life-giving stent. The balloon, which looked more like a tiny test tube than the primary colored toys of your youth you’d imagine, cleared the way for the stent. The stent is used to create a dam or barricade to keep clots from going to the brain.
The patient, alert but mildly sedated, was growing more uncomfortable. “You’re making me anxious in my heart,” Dr. Falatko said. “I know this isn’t easy to sit through.”
Consulting the family just after, she conceded, “It went well, but you know, there’s only so much I can do with tools and medicine. At some point, diet and exercise have to come into the picture, too.” She shrugged a sympathetic shrug and again welcomed questions from the two couches filled with shoulder-to-shoulder loved ones.
noon
On her way to prep for her afternoon surgery, a spinal fusion, a nurse pulled Dr. Falatko in to evaluate another patient. The neurosurgeon is undoubtedly in high demand, currently working all but four days (two weekends) of the month, each month, rotating between being on call for Vascular and Neurosurgery.
While most would describe Dr. Falatko as laser focused, a trait I observed as well, she’s not exactly what you think of when you picture a stereotypical neurosurgeon. She’s absolute but funny, direct but also light when appropriate and mindful of her connection to her patients always.
From Oklahoma originally, Dr. Falatko went to medical school at Oklahoma State University College of Osteopathic Medicine and did her Neurosurgical residency in southeast Michigan at St. John Providence Hospital and Medical Centers. She completed her Cerebrovascular endovascular training at the University of Alabama in Birmingham. The specialties she chose were the only ones that fit, in a way. Nothing else ever seemed to stand out. They never felt right. Her husband, an internist for Parkview, is extremely supportive of his wife’s ambition. “We take it one day at time,” she said when I asked about balance. Though the doctor admits being intentional about more time off is at the top of her list.
1 p.m.
With her slight stature but commanding presence, Dr. Falatko stood at the head of the operating table and applied a clamp to the patient’s skull and neck to keep them still. She directed the team to flip and position the gentleman just so, requesting tools and facilitating last-minute preparations.

Brandon and I stood off to the side in the chilled space, the hairs on my arms standing on end. He explained that the patient had already had a spinal fusion on the front of his vertebrae and now, since they noticed the bones shifted when the patient stood, the area needed to be reinforced by applying screws and rods in the back.
The anesthesiologist, Andrea Waingold, MD, kindly invited me into her area, bordered by screens blinking heart rates and oxygen levels and countless stats she would eye from her seat right next to me. “Just don’t cross into the sterile field,” she cautioned. I leaned ever so slightly forward to watch as Dr. Falatko applied gentle pressure to cut down through layers of firm muscle and tissue. I watched as she applied her weight just enough to secure the screws. Eventually, she would apply a mix of cadaver bone and stem cells, which helps the spine heal within 6 months to a year.
While there was plenty of playful conversation between Brandon, Dr. Falatko and the surgical techs, there was also a palpable stern attention to detail. This patient’s physique required a deeper incision, which made things just a bit more difficult.
A few times she paused and requested a different tool, a different position, a change of this or that. It didn’t come across as a clinician trying to be difficult. It was intuition and confidence. She knew what was right for her as a surgeon and she knew what was right for her patient. No compromising. On multiple occasions during our time together she pulled back the pace and repositioned for precision.
At some point during the procedure she got a call about her stent patient from earlier that morning. Slowly, Dr. Falatko walked over to the speaker phone in the OR and directed his care, step by step, clearly concerned. After they disconnected she stood and collected herself for a few beats before returning to the spinal fusion at hand.
Nearly four hours after we’d walked into the operating room, Dr. Falatko put in the drain and closed up her patient.
5 p.m.
We went to the physician’s lounge so I could change out of my scrubs and I quickly realized this would be my last chance to really chat with Dr. Falatko before we went our separate ways; me back home, her to a department meeting.
“Neurosurgery has such a strong reputation for being a league of the most astute, skilled physicians,” I said, “Do you feel that at all?”
“You know, I don’t. And honestly, you wouldn’t either,” she said, “I deal with so many life and death decisions every day, I don’t think about how I am perceived as a neurosurgeon, a female one at that. In any situation, I know my responsibility is to help that patient in that moment. I don’t feel pressure to be astute and skilled, because it is my job to be those things. That is what people should expect and that is what I strive to deliver. My job is my purpose. I don't feel special, I feel lucky.I get to do something that I love, that can make a difference for people and their families. It's an incredible honor and it humbles me daily."
“I have to ask, is it difficult being a woman in this specialty?”
"I don't care about or get caught up in stereotypes. I have ignored them my entire career. I work hard because it is in my bones to work hard, not because I have something to prove. Plus, there are more women than you think,” she said, the corners of her eyes crinkling from her proud smile. I returned the expression, an unspoken exchange of solidarity, as we walked out of the locker room, me with my backpack, her with her bag, brimming with neurology and vascular texts.

8 p.m.
That night I pulled the red ribbon that marked our spot and began reading about Amelia Earhart. What amazed me about these heroines was the unpretentious nature of their abbreviated biographies. They weren’t trying to make such bold, giant strides. They were simply taking the next step, following the roadmap plotted by intuition, walking toward their fate.
Curious, I turned back to the dedication page. It read:
To the rebel girls of the world:
Dream bigger
Aim higher
Fight harder
And, when in doubt, remember
You are right.



