Rheumatologists specialize in the diagnosis and treatment of systemic autoimmune diseases. These conditions are commonly marked by pain, swelling and stiffness in the joints, but can also impact other organs in the body. According to the American College of Rheumatology, when an individual has an autoimmune disease, their own immune system is attacking their body, which causes inflammation in areas where it’s not needed. We asked Ernesto Levy, MD, Parkview Rheumatology, to explain more about his specialty and why it’s so important to seek treatment as soon as you suspect an issue.
When should a patient see a rheumatologist?
If a patient has specific joint pain, particularly in the hands or feet, that isn’t resolving, the first thing they should do is consult with their primary care provider. They can typically rule out pain that can be addressed through other modalities versus a more systemic issue. If their doctor suspects the patient might have a rheumatic condition, he/she will likely send a referral for the patient to see a rheumatologist for further evaluation and testing.
We can also see patients if they suddenly start experiencing acute joint pain and swelling out of the blue. We can screen the patient to determine if there’s an autoimmune issue. We don’t want patients to suffer longer than they have to, so we recommend seeking care quickly once you notice symptoms outside of typical daily or activity-related discomfort.
Like with other conditions, early intervention produces better outcomes for the patient when it comes to autoimmune diseases. The sooner we can start working on a treatment plan, the less unnecessary pain the patient has to experience.
What kind of tests do rheumatologists do?
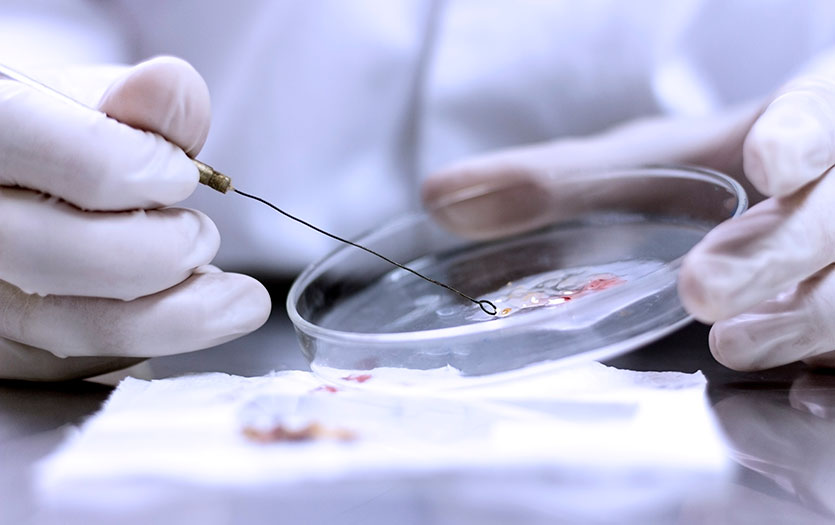
The screening process for autoimmune conditions is generally bloodwork. We will gather a family history and go over your symptoms as well.
With the bloodwork, we are looking for markers of inflammation by checking your C-Reactive Protein (CRP), Erythrocyte Sedimentation Rate (ESR), Anti-Cyclic Citrullinated Peptide (Anti-CCP), and more. This analysis will help us identify any autoimmune disease indicators and also the severity of the condition so that we can prioritize care.
What are the most common autoimmune diseases?
The most common autoimmune conditions we see include rheumatoid arthritis, fibromyalgia, systemic lupus and psoriatic arthritis. But this is not a complete list of the conditions we treat.
Who will be part of my care team?
We really want the primary care provider to be involved, from evaluation to referral and throughout the treatment process. We can’t screen people for autoimmune conditions over the phone, so we really rely on physicians to identify potential issues and bring them to our attention, particularly if the patient has indicators of autoimmune disease.
Depending on the condition, we might need to manage it in tandem with other specialties. A rash, for example, can be a symptom of autoimmune disease. If a patient is experiencing issues with their skin as a result of their condition, we would work alongside Dermatology to treat the patient and manage their symptoms.
And it’s important to mention that the patient is an integral part of the care team. We are typically dealing with chronic, long-term diseases, so we have to work for quite a few months before we establish the most helpful treatment. Up until that point, there’s a lot of adding and adjusting medications to find what will work best. We partner with the patient to determine what’s next. Yes, I’m the doctor, but I want to hear the patient’s opinions, concerns and descriptions of what they’re experiencing so that we can manage the disease together.
Parkview Health has rheumatology providers on the Parkview Regional Medical Center campus. If you're interested in establishing care with one of our providers, speak with your primary care provider about your concerns or call our 24/7 scheduling center at (877) PPG-TODAY.