This post was written by Josh Haddock M, MB(ASCP), Microbiology Specialist, Parkview Health.
Antibiotic resistance has become one of the most significant challenges in modern medicine. Understanding how it works at the microbial level helps explain why it deserves serious attention—not just in hospitals and research labs, but in everyday life.
What happens inside an infection
Bacteria are living organisms with a remarkable capacity to adapt. When a bacterial infection takes hold, and antibiotic treatment begins, the medication eliminates most bacteria in the population. However, within any large bacterial population, some cells carry small genetic variations that make them slightly harder to kill. Those cells survive, replicate and pass their resistance traits to the next generation.
This is the process that microbiology laboratories observe directly. When a clinical sample is cultured and tested against a panel of antibiotics—a standard procedure called susceptibility testing—each result reflects the real-world status of the bacteria causing a patient's infection. Increasingly, those panels return results showing reduced sensitivity or outright resistance, meaning drugs that worked reliably a decade ago may no longer stop the same infections today.
How laboratories measure and track resistance
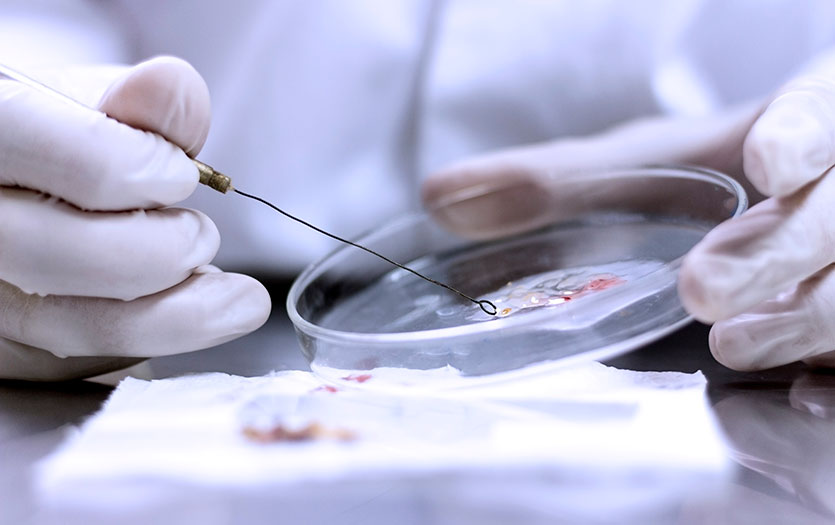
When a patient sample arrives in a clinical microbiology laboratory, scientists grow the bacteria it contains under controlled conditions and then systematically test how different antibiotics perform against that specific strain. Two methods are central to this work.
In disk diffusion testing, small paper disks soaked in individual antibiotics are placed on a plate where bacteria are growing. After incubation, the size of the clear zone surrounding each disk—where bacterial growth has stopped—indicates how effectively the antibiotic works.
The other approach measures what is called the minimum inhibitory concentration (MIC), which is the lowest concentration of an antibiotic that prevents visible bacterial growth. Together, these methods give clinicians a precise picture of what is and is not working.
The lab reports these results back to the treating physician in straightforward terms: a bacterium is classified as susceptible, intermediate or resistant to each drug tested. A susceptible result means standard dosing is likely to clear the infection; a resistant result means that the antibiotic should not be used. These categories directly shape prescribing decisions, often within hours of a sample being collected.
Over time, individual test results become something more. Hospitals compile resistance data from all patients tested over a given period into a summary document called an antibiogram. This report shows at a glance which antibiotics remain reliably effective against the most common organisms in that facility. Before a specific patient's results are back, physicians can consult the antibiogram to make an informed initial choice, which is an important advantage when starting treatment quickly matters.
Beyond the hospital, laboratories contribute their data to national and international surveillance systems. In the United States, facilities report to the Centers for Disease Control and Prevention's (CDC) National Healthcare Safety Network (NHSN), which monitors resistance trends across thousands of healthcare settings. Globally, laboratories in more than 90 countries use WHONET, a software developed by the World Health Organization (WHO) to standardize how resistance data is recorded and shared. This collective picture allows public health authorities to detect emerging outbreaks, identify new resistance patterns as they spread, and shape antibiotic policy at the hospital, national and global level.
Why unnecessary use accelerates the problem
Antibiotics are effective only against bacteria, not viruses. Viruses cause colds, influenza, and most cases of sore throat. Antibiotics do not affect these illnesses. Taking antibiotics in these situations does not provide therapeutic benefit. It does, however, apply selective pressure to the bacteria naturally present in the body. The tougher, more resistant strains are the ones most likely to survive that pressure and persist.
Finishing a full course of antibiotics is equally important. Even when symptoms improve after a few days, bacteria may still be present in the body at lower numbers. Stopping early leaves the hardiest, most resistance-prone cells alive. Those survivors can rebound, cause a second infection that is harder to treat and spread to others. Completing the full prescribed course ensures the antibiotic clears the bacterial population as thoroughly as possible, reducing the chance that resistant strains are left behind to multiply.
The cumulative effect
Resistance does not develop in isolation. Resistant strains move between individuals, between communities and across healthcare settings. What begins as a single interrupted prescription or an unnecessary course of antibiotics contributes to a broader pattern that is visible in lab data across hospitals and public health surveillance systems worldwide.
When questions arise about whether an antibiotic is appropriate or how to take a current prescription, a treating clinician or pharmacist is the right resource. The science of susceptibility is complex, but the underlying principle is straightforward: these medicines work best when used precisely, and their long-term effectiveness depends on exactly that.
To learn more about Parkview's laboratory services, visit us here.


.jpg)
